Plastic Surgery Camp October 2015 (Nigeria)
Cees Spronk, Plastic surgeon, leader of the team
Peter Houpt, Plastic surgeon
Robbin Thieme Groen, Anaesthesiologist
Geke Hoeksma, Anaesthesia assistant
Geesje Bonhof, Anaesthesia assistant
Fatima van Klaveren, Operation assistant
Sandra van der Broek, Operation assistant
Marthe Houpt, Communication advisor
Neeltje Spronk- Mulder, Deputy Fardipur foundation
Ellen Meerman, Trainee Plastic surgeon (author of the report)
Hospital: COCIN Hospital and Rehabilitation Centre, Mangu
It took a long time before all the visa were okay. Eventually we could collect our passports and visa on the day of departure at Schiphol, but a day before departure we were told that three passports were missing. Fatima, Geesje and Marthe cannot travel together with us, so on Saturday morning we travel from Schiphol via Frankfurt to Abuja with an incomplete team. Cees and Neeltje had left a week earlier to Mangu. At the airport everything goes smoothly. We were asked if we had medicines. We had, but only for our own use. Sandra shows the Customs Officer the packing list and then we can move on without even having to open our suitcases. Cees, Kefas and two drivers meet us and we continue our trip by bus. After one night in Abuja it takes us six hours to reach Mangu the next day. The crowded dual carriage way of Abuja does not seem to have any traffic rules apart from the one that drivers who blow their horns loudest seem to have right of way. After some time we reach the quieter roads of Plateau State. Every now and then we reduce speed for a road block, where soldiers with arms let us pass without asking questions. On Sunday afternoon we arrive in Mangu. Neeltje meets us in the newly built guesthouse (financed by the Fardipur foundation), where Phoebe has prepared a delicious dinner. We are glad that the trip went well.
On Monday morning a rooster wakes us. Life in Mangu starts early, when the sun comes up. In the operation theatres, where everything is covered in dust a part of the team begins with cleaning and unpacking the suitcases that we brought from Holland. Each person has two suitcases of 23 kilos each, which we packed with operation material, stitches and bandages. The doctors of the team go to the policlinic, where people queue to be selected for the operation. This ‘screening’ takes the rest of the day. One by one the patients are seen by Peter or Cees, and later by Robbin. Patients who can be operated are put on a list and get a date when to return. With most patients we can communicate well in English. Cees manages to speak some Housa and if we miscommunicate Kefas or het nurses translate. I weigh the patients and make X-rays. I’m deeply impressed by the many small children with burns contractures in several stages. I cannot image how much pain these children must have suffered. We see patients of all ages with several types of schisms. I have to get used to this, because in Holland all split lips are closed before the age of one year old. We see boys with hypospadias and some patients with sexual ambiguity, a few other congenital deformities such as syndactylism, duplication of fingers and macrostomia. And we see patients with tumours, sometimes enormously big, among which a number of neurofibromes (benignant but destructively growing tumours) and many keloids (the abundant growth of scar tissue).

Long queues for the screening
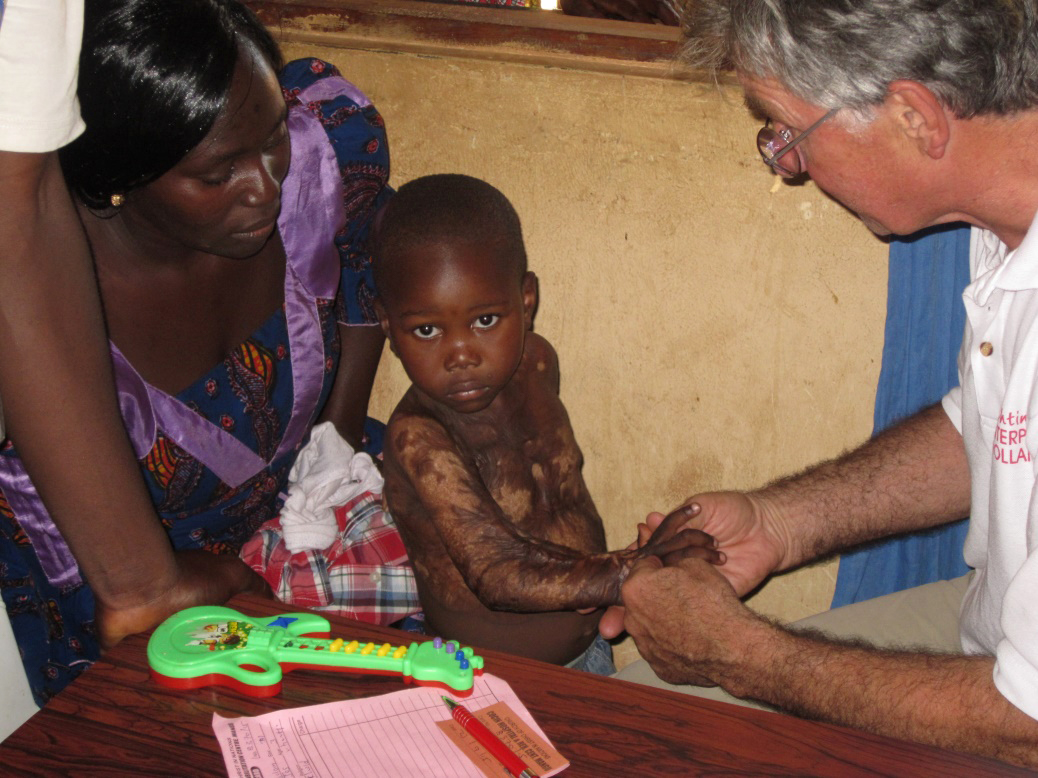
Cees sees one of the many patients with burns contractures
The first operations are planned for the next day. At first this is exciting: does all the equipment function properly and how is the cooperation with the new members of the team? Fortunately everything goes well. A power cut causes some panic as the anaesthesia machine gives no oxygen, but after manual respiration the power machine is switched on and the operation could be completed successfully. In the evening there is good news: Fatima, Geesje and Marthe were given temporary passports with visa. They can leave on Wednesday and so on Thursday the entire team is complete in Mangu.
We work long days and operate on average 11 patients a day on two tables simultaneously. At the end of the day there are often patients waiting to be operated upon. Because of the large number of patients we also operate on Saturday and on the last Friday that originally was meant for inventory and packing. Not all patients can be operated upon; some will have to return next year.
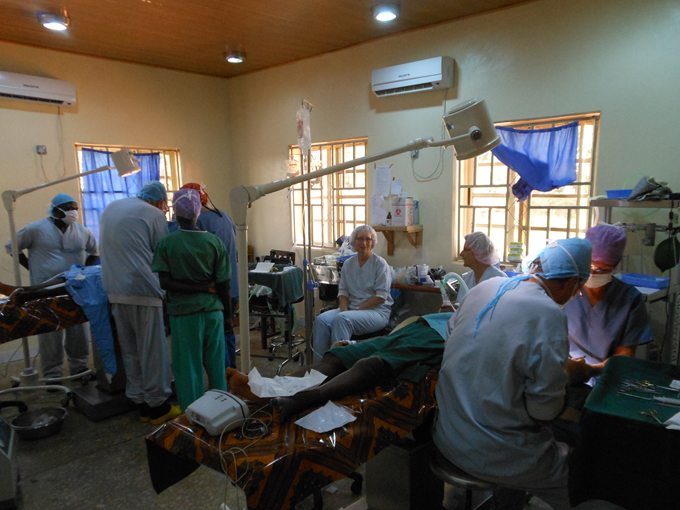
Two operation teams working simultaneously
The operation theatres are busy. Besides our own team the local team works hard. Instruments are put in the autoclave, the tables are made in order, equipment is handed over and patients are shown in and out. Local doctors, who regularly take a look and make X-rays, or even assist when washing patients show much interest. Nurses and the physiotherapist also know where to find the operation theatres and check our work regularly.
We operate upon patients with beautiful names such as Happy Jerry, Friday Justice, Marvellous Monday, Ambitions Rehop and Ponfa Goodness. All patients are given a small present. Children receive small bears or cars; adults receive a pen or a key-cord. When we visit the ward to check the patients we see how happy the younger patients are with their presents: a girl carries her new bear in a shawl on her back just like mothers are used to carry their babies here. Whereas many mothers like their photos taken together with us, the younger patients still find the doctors in white scary. Changing the bandages is often accompanied by tears. As a reward for their courage we hand out balloons, which are accepted gladly.
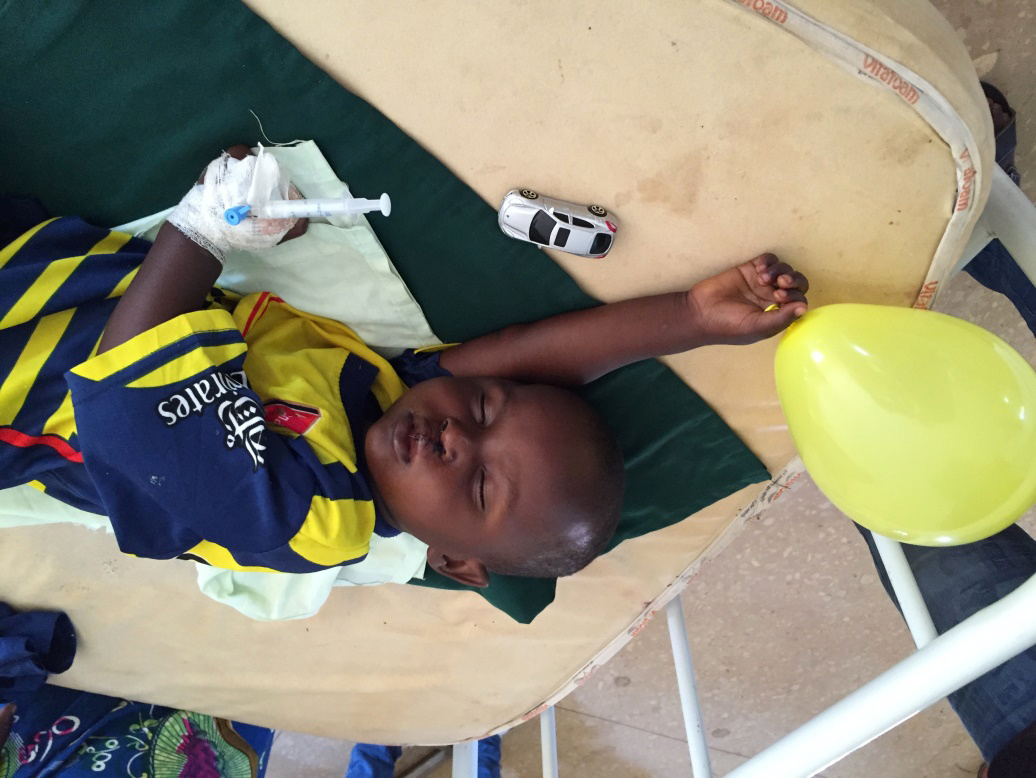
A sleeping boy on the ward after closure of his lip, proud of his car and balloon
Twice a day Phoebe prepares a delicious meal for us in the guesthouse. In the evening there is some time for relaxation: we read books or play Machiavelli. On Sunday we visit a local church and stroll along the river.
In the second week time is again flying. Before we know it is Friday, the last day when we do operations. Peter waited with a special patient for this day: a man with a gigantic keloid of his chin, an abscess reaching to his umbilicus: literally a splashing end. During this mission we operated upon an absolute total of 105 patients, of whom 73 children and 32 adults. We saw 59 patients with burns contractures, 14 patients with urogenital problems (such as hypospadias) and 9 patients with schisms.
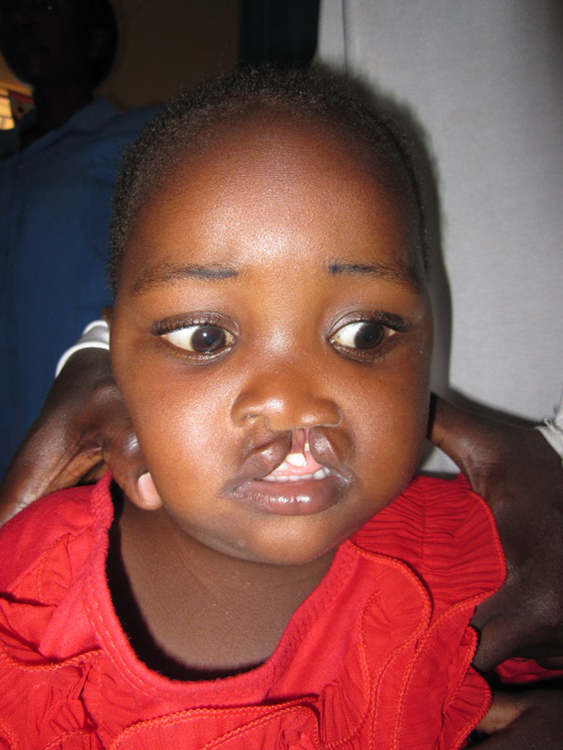
Girl before lip closure

Same girl one day after the operation
Besides the operations we also paid much attention to the prevention of burns during this mission. Marthe helped Kefas making a ‘Burns prevention Programme’. Many children contract burns while playing when their mothers prepare food using pans on an open fire with three stones on the ground. To show the dangers of the open fire Marthe and Kefas gave presentations and taught pupils, patients and their parents. To underline this posters and torches were made showing information to prevent burns and how to treat them. The pupils and the patients’ parents reacted enthusiastically. Some creative people made special ovens from clay on which dinner can be cooked without an open fire. Hopefully these efforts result in a successful continuation of the Burns Prevention Programme, so that during the next missions fewer and fewer burns contractures have to be operated.

Making clay ovens
Traditionally on the last Friday evening there is a dinner with the staff, doctors and head nurses of the hospital. Words of gratitude are spoken and we take leave, although that is for the time being, because there is a new list of patients that need operations in 2016. After a good journey home we all look back on a very successful mission.
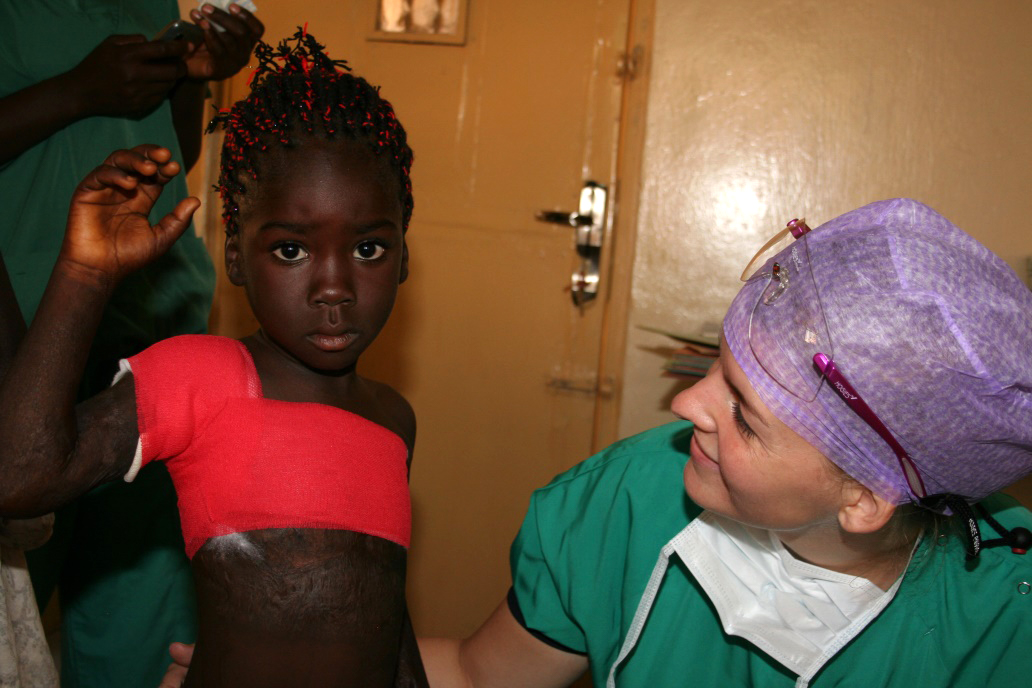
This girl can lift her arm again and wave after an operation of her burns contracture in her armpit

